- Al-Hussain Business Park, Jordan
- +(962) 000-0000
- info@curafile.com
Skin Lupus
- Home
- Skin Lupus
Cutaneous lupus is one type of lupus — an autoimmune disease that causes inflammation in different body tissues. “Cutaneous lupus,” which means skin lupus, affects your skin. Inflammation in your skin causes a variety of symptoms — most often a red, scaly rash. These symptoms are triggered by sunlight exposure. Medications can treat them.
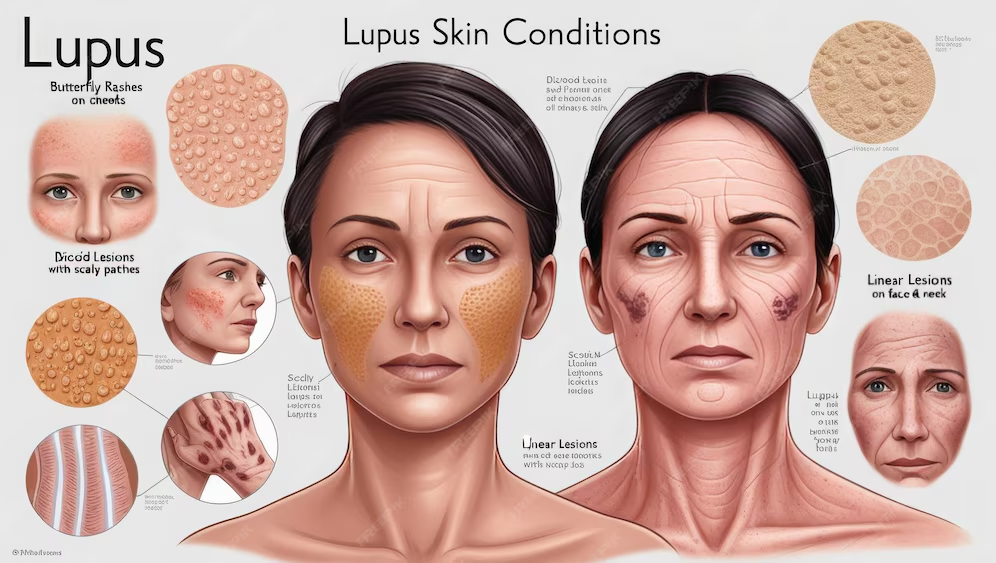
Cutaneous lupus erythematosus is an autoimmune disease. This means your immune system causes your symptoms. Your immune system generates antibodies that target certain proteins in your body. This usually works to defend you from disease. But in autoimmune disease, your immune system mistakenly targets your own body tissues. This causes the ongoing inflammation in your skin.
Scientists still don’t understand everything about why this happens. They believe it’s a combination of factors. Certain genetic variations make you more likely to get the disease. Then, certain environmental factors can trigger it. These environmental factors provoke a stress response from your immune system. UV radiation exposure (fluorescent light or sunlight) is the most important trigger of cutaneous lupus.
Red, scaly areas of skin. They might look like a coin or a ring. They especially occur on sun-exposed areas. Rashes might appear purple or brown on darker skin tones.
A red rash that spreads across your cheeks and the bridge of your nose, in the shape of a butterfly (malar rash). Rashes might appear purple or brown on darker skin tones.
Patches of lighter and darker pigment on your skin. These are the remains of lesions that have healed.
Photosensitivity (skin symptoms worsen with UV light exposure).
Skin itching or irritation.
Skin swelling (edema), especially around your eyes.
Hair loss related to scarring on your scalp.
Mouth sores or sores inside your nostrils.
Other possible symptoms include:
- Hives.
- Livedo reticularis.
- Raynaud’s syndrome.
- Spider veins.
- Petechiae.
- Red palms.
If you develop lupus skin symptoms, consult a dermatologist familiar with lupus. They’ll ask about your symptoms and examine your skin. Some lupus rashes are recognizable on sight, but others are less recognizable or resemble other skin conditions. Your provider might need to take a small skin sample to examine under a microscope (skin biopsy). If necessary, they might conduct further tests, including:
Direct immunofluorescence (lupus band test). This test examines your skin biopsy sample under a fluorescent microscope. They look for a band of tagged antibodies in the sample.
Blood tests. Your provider may conduct blood tests to screen for systemic lupus. While blood tests alone can’t diagnose lupus, they can detect certain signs, like antibodies related to SLE.
There isn’t a cure for CLE, or any autoimmune disease. But medications and lifestyle changes can help reduce your symptoms. For example, limiting your sun exposure can help minimize skin reactions. Treating your skin with medications can help soothe skin reactions when they arise. Your healthcare provider will prescribe treatments based on your symptoms and the type of skin lupus you have.
How do healthcare providers treat cutaneous lupus?
Your provider may recommend:
Limiting sunlight exposure: Learn to stay inside when the sun is strongest during the day. Wear a wide-brimmed hat, sun-protective clothing and sunscreen when you can’t avoid the sun.
Vitamin D supplements: Limiting your sunlight exposure can put you at risk of vitamin D deficiency. Your provider will monitor your levels and prescribe supplements if necessary.
Topical medications: Creams, lotions and ointments can reduce skin inflammation. You may need to apply these daily. Corticosteroid creams and tacrolimus ointment are two examples.
Injections: Your provider may inject a corticosteroid medication directly into your rash. Steroid injections help reduce inflammation and pain. You may need these injections every few weeks.
Oral medications: Disease-modifying anti-rheumatic drugs (DMARDs) treat autoinflammatory diseases like lupus. Hydroxychloroquine and chloroquine are most often prescribed for CTE.
Having a female reproductive system, especially during periods of high estrogen.
Having African American heritage.
Having certain genes that are common in people with lupus.
Having another autoimmune disease.
Severe stress to your immune system (like a serious illness or injury).
Prolonged use of certain medications.
Prolonged sun or UV light exposure.
Smoking.
Cutaneous lupus is a lifelong condition. But with medical treatment and lifestyle changes, you can learn to manage your symptoms. What your symptoms are like, which treatments work best and how well they work can vary from person to person. Unlike systemic lupus, cutaneous lupus doesn’t cause life-threatening symptoms. It shouldn’t affect your life expectancy. But it can affect your quality of life.
Cutaneous lupus can manifest in different ways. For some people, symptoms appear and disappear suddenly. For others, they go on indefinitely, getting better or worse. Cutaneous lupus can also cause different skin lesions with different characteristics. Many of these only occur with lupus. Healthcare providers classify skin lupus by how often you have symptoms and the types of skin lesions you have.
Chronic cutaneous lupus
Chronic CLE causes steady skin symptoms, which may get better or worse but never go away completely. The lesions it causes may leave permanent scars or skin discoloration.
Subtypes include:
- Discoid lupus.
- Lupus profundus (lupus
- panniculitis).
- Chilblain lupus.
- Lupus timidus (intermittent cutaneous lupus).
Acute cutaneous lupus
Acute CLE is a lifelong condition, but the symptoms occur in an acute manner. That means they come on suddenly and then disappear for a while. It doesn’t tend to leave scars.
ubtypes include:
- Localized ACLE (malar rash).
- Generalized ACLE (maculopapular rash).
- Toxic epidermal necrolysis-like ACLE.
Subacute cutaneous lupus.
Subacute CLE occurs for limited periods, but repeatedly. For example, it may return every summer with sunlight exposure. It affects a deeper layer of skin, below the epidermis.
Subtypes include:
- Annular SCLE.
- Papulosquamous SCLE.
systemic lupus erythematosus (SLE).
References
- American Academy of Dermatology Association. Lupus and Your Skin: Overview (https://www.aad.org/public/diseases/a-z/lupus-overview). Updated 9/23/2022. Accessed 10/25/2024.
- Arthritis Foundation (U.S.). Cutaneous Lupus Symptoms and Treatments (https://www.arthritis.org/diseases/more-about/cutaneous-lupus-symptoms-and-treatments). Accessed 10/25/2024.
- Little AJ, Vesely MD. Cutaneous Lupus Erythematosus: Current and Future Pathogenesis-Directed Therapies (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7087060/). Yale J Biol Med. 2020 Mar 27;93(1):81-95. Accessed 10/25/2024.
- Lupus Foundation of America. Lupus and Skin Rashes (https://www.lupus.org/resources/lupus-and-skin-rashes). Updated 2/8/2024. Accessed 10/25/2024.
New Zealand Dermatological Society. Cutaneous lupus erythematosus (https://dermnetnz.org/topics/cutaneous-lupus-erythematosus). Accessed 10/25/2024. - Okon LG, Werth VP. Cutaneous lupus erythematosus: diagnosis and treatment (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3927537/). Best Pract Res Clin Rheumatol. 2013 Jun;27(3):391-404. Accessed 10/25/2024.
Related Topics
Good Habits You Should Know
Bad Habits You Should Know
-
Find a clinic near you
-
Call for an appointment!
-
Feel free to message us!
About Us
Curafile is the biggest Healthcare Curated Network Globally that serves citizens, service providers in one place.
- Al Hussain Business Park
Amman, Jordan

